MEET THE SURGEON

Dr Libby Anderson, BCom BSc MBBS FRACs FAOA
Subspecialist Orthopaedic Hand & Wrist Surgeon
Public and Private Practice
Active in Research & Academic Teaching
Special interest in trauma, nerve compression syndromes and management of carpal instability
OVERVIEW
19 year-old right-hand dominant male student presented with right wrist stiffness, weakness and pain at the extremes of motion and on palpation of the dorsal lunate.
X-ray and CT indicated a dorsal lunate fracture with an established non-union. Dr Anderson elected to perform a lunate Open Reduction Internal Fixation (ORIF) with a FO 1.5x12mm microscrew.
CASE INTRODUCTION
19-year-old right-hand dominant male student presented with right wrist stiffness, weakness, and pain at the extremes of motion. Imaging indicated a dorsal lunate fracture with established non-union.
CASE PRESENTATION
Patient presented with insidious onset of right wrist pain, gradually worsening during football practice. Over the course of several months, this progressed to stiffness and weakness, and worsening of pain at the extremes of motion. On examination, the patient had tenderness on palpation of the dorsal lunate. X-ray and CT indicated the presence of a dorsal lunate fracture with an established non-union. The articular surfaces were well preserved. The scapholunate interval was normal. Carpal alignment was otherwise within normal limits.
PRE-OPERATIVE PLAN
As there was absence of degeneration, Dr Anderson elected to perform an ORIF, utilising the FO 1.5mm Microscrew. This implant was selected due to the required strength of the construct and the delicate nature of the fragment. It was considered that the FO Microscrew was the most appropriate implant for this procedure primarily due to its cannulation, the scale of the screw, and its reliability in compression.
Below: Pre-Operative Imaging


SURGICAL APPROACH
A dorsal midline skin incision was made and an approach to the lunate was undertaken in the line of the dorsal radiocarpal (DRC) ligament fibres. Once on bone, the chronic non-union of the lunate was identified. The fragment was assessed and found to be predominantly cartilaginous with a small amount of bone, enough to take a FO Microscrew. The fragment had attachments to the lunotriquetral and scapholunate ligaments. Intraoperative examination showed the scaphoid and lunate proper moved as one. It was concluded that the preoperative plan would be appropriate.
Operative site preparation
The lunate was debrided using a curette. The fragment, which was small and predominantly cartilaginous in nature, was sharply derided using a blade. Careful consideration was taken not to remove too much bone as well as to preserve the ligamentous attachments.
Graft Harvesting
To improve the chances of success, bone graft was taken from the right distal radius, by creating a bone trap-door cortical window and curetting out cancellous bone from Lister's tubercle.
Reduction
Reduction was achieved by capturing the bony cartilaginous fragment with the 0.6mm FO k-wire. Once inserted,the k-wire was used to control the delicate fragment and joystick it into place. The k-wire was then driven through into the lunate, achieving and securing the temporary reduction.
Implant selection
As unicortical fixation of the lunate was aimed for in this case, intraoperative imaging was used to ensure appropriate k-wire length. The k-wire was then measured with the FO depth gauge to determine the appropriate implant size. In this case, an implant of 1.5 x 12mm was determined to be suitable.
Definitive fixation
Once the appropriate implant was selected, definitive fixation was performed in the standard manner. As the lunate is delicate, Dr Anderson elected to hand drill, utilising the FO 1.1mm drill bit. It was considered that the ergonomics of the FO handle enabled suitable control and ease of use for precise and accurate drilling. Once drilled, the pre-harvested bone graft was packed between the lunate and the fragment. The 1.5 x 12mm FO Microscrew was then inserted over the k-wire to achieve definitive fixation. The fixation was solid and stable through wrist range of motion. There was no impingement of the screw dorsally. The wound was irrigated, and appropriately closed in layers. The patient was temporarily immobilised in a volar slab for comfort.
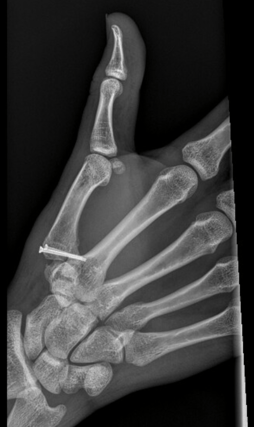
Below: Intra-operative fluoroscopic images


FOLLOW UP
The patient was changed from a volar slab to a thermoplastic wrist splint day 1 post surgery. He remained in this splint full time until union was confirmed on CT scan. Partial union was achieved at 8 weeks post-op and complete union at 12 weeks post-op. After confirmation of union, the patient was further treated by hand therapy and allowed to go out of the splint to start active and passive range of motion to address stiffness and return to normal quality of life. At 4 months post surgery, the patient had a grip strength of 36kg, which was equal to his contralateral side. He had no pain and could achieve wrist flexion and extension of 60 degrees.
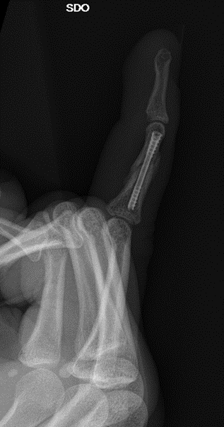
Below: Post operative images

DISCUSSION
The cannulated advantage of the Microscrew system contributed to the success of this operation. The cannulated design of the system makes it extremely easy to use and the patented head design of the screw provides impressive compression. Once reduction was achieved, there were no further issues with fragment management and the bone was able to be prepared and definitively fixed without loss of reduction. Furthermore, due to the small scale of the implant and the graduated taper of the head of the Microscrew, this small fragment was able to be definitively and reliably fixed. The head was able to reduce and hold the fragment stable without risking shattering of the dorsal fragment.
The management of small and fragile fractures and fragments has always been a complex and tricky procedure. Reducing fragments and achieving definitive fixation with an implant small and strong enough has always been a challenge. The FO Microscrew system has become my go-to solution for the management in small and complex fractures and fragments of the distal extremities.