MEET THE SURGEON

Dr. Jordan Grier, MD
- Orthopaedic Surgeon at OrthoCarolina, Charlotte North Carolina
- Specializing in upper extremity (Hand, Wrist, Elbow, and Shoulder)
- Medical Degree and Residency Training, Duke University Medical Center
- Subspecialty Training, OrthoCarolina Hand Center
DISCLAIMER
The opinions expressed by Dr. Grier are those of Dr. Grier and not necessarily those of Field Orthopaedics. Individual experiences may vary.
The procedure described in the report may differ from the manufacturer’s surgical technique. Surgeons are advised to review the product specific surgical technique prior to performing any surgery.
A surgeon must always rely on their own professional clinical judgement when deciding whether to use a particular product when treating a particular patient. A surgeon must always refer to the instructions for use, product label and surgical technique before using any Field Orthopaedics product. Product may not be available in all markets. Please contact your Field Orthopaedics representative if you have any questions about availability of Field Orthopaedics products in your area.
OVERVIEW
A 56-year-old female presented to Dr Grier after sustaining an injury to her left hand while riding an E-bike. Radiographs confirmed a spiral fracture of the fourth metacarpal diaphysis with displacement in both the coronal and sagittal planes.
With a desire to return to her active lifestyle and a concerning degree of malrotation present, the decision was made to stabilise the fracture with an NX Nail from Field Orthopaedics. At follow-up the patient demonstrated full active range of motion of the ring finger, was able to make a fist and had all motor function intact. With preserved implant alignment and no evidence of hardware failure, the patient was able to resume normal function without restriction.
CASE INTRODUCTION
A 56-year-old right-handed female Marketing professional, presented to Dr Grier for evaluation of a closed fracture of the fourth metacarpal after she sustained a direct blow to her left hand when her E–bike unexpectedly activated. As a recreationally active individual, she was keen to return to active use of her hand as quickly as possible.
CASE PRESENTATION
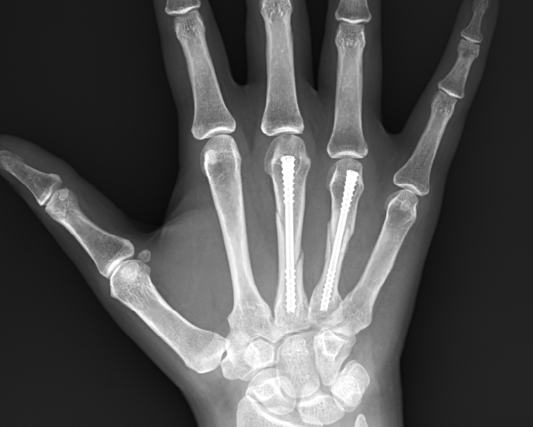
At the time of injury, the patient had immediate onset of pain and swelling around the ulnar aspect of the hand. Radiographs confirmed a spiral fracture of the fourth metacarpal diaphysis with displacement in both the coronal and sagittal planes (shown below).
Below: Pre-Operative Imaging



Upon examination, the left hand had significant swelling and associated bruising dorsally and in the palm. Flexion and extension of the fingers and wrist was limited by pain and the hand was tender over the fourth metacarpal. The patient reported having pins and needles to the tips of all fingers and had a mild malrotation of the ring finger with active flexion. Prior to the injury, the she had no pain, disability, tingling or weakness in her left hand.
PRE-OPERATIVE PLAN
Surgical and non-surgical treatment options were discussed with the patient. While Dr Grier expected the fracture to heal with appropriate nonsurgical management includinXg closed reduction and splinting, he was concerned about the degree of malrotation (approximately 7 degrees) present upon examination. The patient was made aware that should the fracture heal in a malunited position, it could cause long-term disability and displeasure with her hand function. While a corrective osteotomy could address this in the future, the associated risks, benefits, expected recovery and outcomes were unfavourable. Additionally, the patient’s primary desire was to return to exercise, high-level tennis, and normal activities around her home as quickly as possible.
As with other fractures the intent for treating high energy wrist injuries involves restoring length and alignment, whilst attempting to obtain congruency of the articular surface, particularly of the radiocarpal and distal radioulnar joints. Unfortunately, unlike simpler fracture patterns, high energy injuries are often associated with extensive articular surface comminution and extension into the radial diaphysis, as was the situation in this case.
For these reasons, the decision was made to proceed surgically with anatomic reduction of the fracture and definitive fixation with an NX Nail from Field Orthopaedics to get her moving again and reduce the risk of long-term malrotation of the ring finger. As the NX Nail has been designed with an anatomically inspired head, increased distal engagement and a non-compressive design (based on the AO principles of fracture management), it was considered to provide stability, allow rapid return to function, and reduce the risk of deformity.
SURGICAL APPROACH
The patient presented for Open Reduction Internal Fixation six days after the initial injury.
Reduction
Fluoroscopic images of the left hand demonstrated a closed, displaced, spiral fracture of the mid-diaphysis of the fourth metacarpal. The fracture was reduced using manual traction and force applied perpendicular to the fracture site to provide anatomic reduction in both coronal and sagittal planes.
Bone Preparation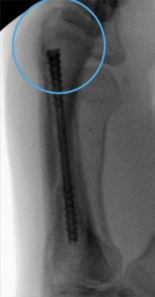
A guidewire was placed percutaneously in the distal metacarpal at the level of the metacarpal head. Intraoperative fluoroscopy was utilised to advance the guidewire in a retrograde fashion into the medullary canal, across the fracture site, into the base of the fourth metacarpal and confirm anatomic reduction and desired guidewire placement. A 1cm incision was made over the guidewire at the distal aspect of the metacarpal. The corresponding drill for the 3.0mm Field Orthopaedics NX Nail was used to drill over the guidewire via the open incision.
Note: the desired placement of the entry portal within the dorsal portion of the Metacarpal head.
Definitive Fixation
After the appropriate path for the nail had been created, a 3.0mm x 45mm NX Nail was inserted in a retrograde fashion over the guidewire with careful attention paid to maintenance of the anatomic reduction of the fracture site. Correct implant placement was confirmed with fluoroscopy and rotation of the finger carefully scrutinised and noted to be anatomic relative to the cascade of the adjacent digits as well as her contralateral unaffected hand. Normal tenodesis of the digital flexors and extensors of the ring finger was noted.
Below: Intraoperative Imaging



Closure
The wound was irrigated with saline and closed with a 4-0 nylon suture in a horizontal mattress fashion before being dressed with sterile Xeroform, 4x4 gauze, cast padding and a well-padded ulnar gutter P1 block splint applied.
Post-Operatively
The patient was advised to spend three days in the postoperative splint with active range of motion of the fingers within the confines of the splint encouraged immediately.
FOLLOW UP
Two Weeks
At her two-week follow-up appointment, the patient reported some transient pain at the fracture site overnight.
One Month
By one month the pain reported at two-weeks had resolved and the patient had no other pain and was no longer using a splint or other orthosis.
Examination of the left hand showed a well-healed incision, full active range of motion of the ring finger, the ability to form a full fist and all motor function intact throughout the extremity. X-rays showed preserved implant alignment and no evidence of hardware failure. The patient was advised to continue using her hand for all activities as tolerated without restrictions.
Two and a Half Months
At her final follow-up appointment, the patient reported having no pain and had returned to competitive tennis and weightlifting without issue. While she reported some mild subjective stiffness in her fingers, objectively she was able to make a full composite fist. The patient was happy to continue working on range of motion exercises at home without formal therapy.
Below: Post-Operative Imaging at Two and a Half Months



DISCUSSION
In this case, Dr Grier was able to achieve an excellent outcome for an active patient who was motivated to resume her normal activities as soon as possible. Surgical intervention allowed for correction of the malrotation deformity and provided the patient with a superior alternative to a conservative approach.
With the NX Nail Dr Grier was able to rigidly fix the head and base fragments in space whilst crossing the fracture to stabilise the key bone structures in the anatomic position supporting restoration of native biomechanics. With an anatomically inspired tapered head, narrow waist and cutting efficiency, the NX Nail is engineered to provide increased engagement and fragment control to achieve rigid stability and true fixation. Facilitated by the strength of Titanium Ultra- Alloy, there is no need for isthmus stuffing or maximising implant length to achieve subcortical engagement. All that is required is to select an implant long enough to cross the fracture and wide enough that the surgeon is satisfied with the head purchase.
FO-003267-MM Version 2 April 2025