MEET THE SURGEON

Professor Greg Couzens, FRACS(Orth)
Fellowship trained Orthopaedic Hand Surgeon Brisbane, Australia.
Researcher at the Institute of Biomedical Health and Innovation at the Queensland University of Technology.
DISCLAIMER
The opinions expressed by Prof. Couzens are those of Prof. Couzens and not necessarily those of Field Orthopaedics. Individual experiences may vary.
The procedure described in the report may differ from the manufacturer’s surgical technique. Surgeons are advised to review the product specific surgical technique prior to performing any surgery.
A surgeon must always rely on their own professional clinical judgement when deciding whether to use a particular product when treating a particular patient. A surgeon must always refer to the instructions for use, product label and surgical technique before using any Field Orthopaedics product. Product may not be available in all markets. Please contact your Field Orthopaedics representative if you have any questions about availability of Field Orthopaedics products in your area.
OVERVIEW
A 20-year-old female professional Australian Football League (AFLW) player suffered an injury to the ring finger of her dominant right hand in a collision at training. She was seen by Prof. Couzens the next day and presented with pain, swelling and an angulated finger. Radiographs showed a comminuted fracture of the middle P2 phalanx.
ouzens achieved definitive fixation with a 2.0mm x 22mm NX Nail through a percutaneous approach. The operative finger was buddied to the middle finger initially and the patient was seen by a hand therapist for provision of a training and playing splint. By six weeks she was cleared to return to contact ball work with no restrictions in the gym. In this instance, Prof. Couzens was able to treat a painful and debilitating injury for a young patient whose vocation requires the full use of her hand and fingers.
CASE INTRODUCTION
A 20-year-old female professional Australian Football League (AFLW) player suffered an injury to her right ring finger in a collision at training. As a young professional athlete and part-time retail assistant with an injury to her dominant hand, rapid return to full function was the highest priority.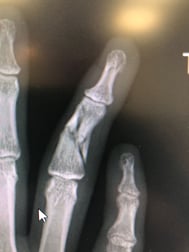
CASE PRESENTATION
The day after sustaining the injury, the patient was seen by Prof. Couzens. Upon examination, she had pain, swelling and an angulated finger. Radiographs showed a comminuted fracture of the middle P2 phalanx of the right ring finger.
PRE-OPERATIVE PLAN
To facilitate a rapid return to function, Prof. Couzens planned for definitive fixation with an NX Nail through a percutaneous approach. This minimally invasive approach would allow him to realign and stabilise the fracture with limited disruption to surrounding soft tissues. Hand therapy would also be required to mobilise the finger post-operatively so the patient could return to training in stages as she progressed through her recovery.
SURGICAL APPROACH
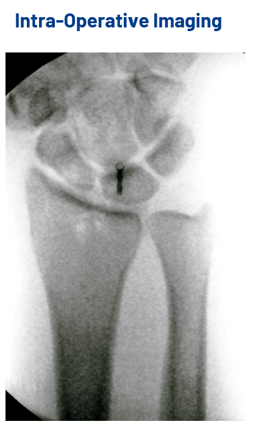
Under intra-operative fluoroscopy, the fracture could be reduced with traction.
Below: Intra-operative Imaging


Once realigned, Prof. Couzens passed a 0.8mm K-wire across the fracture to temporarily hold it in place before using a cannulated drill to prepare for the implant.



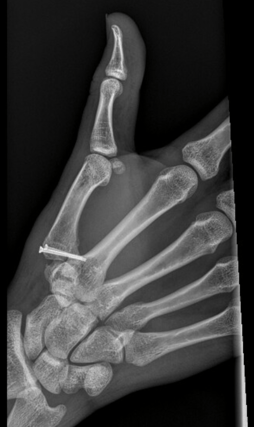
A 2.0mm diameter NX Nail which was 22mm in length was used to stabilise and fix the fracture. Implant placement was confirmed under fluoroscopy before the guidewire was removed and the small incision closed with a 5-0 suture. The operative finger was buddied to the middle finger initially and she was seen by a hand therapist on the first post operative day for provision of a training and playing splint.
Below: Intra-operative Imaging




FOLLOW UP
Two weeks post-operatively, the incision site had fully healed and the patient was doing exceptionally well. She did not report any significant pain and her swelling had resolved. She was rapidly recovering her range of motion and was provided with a resting splint due to a tendency for mild swan neck deformity.
At five weeks, the patient was progressing well with her range of motion in hand therapy and had minimal swelling at P1 and P2 of the right ring finger. Range of motion at the proximal interphalangeal joint was from 5o of hyperextension to 100o of flexion. At the distal interphalangeal joint range was from -5o of extension to 50o of flexion. During the day the operative finger was buddy strapped to facilitate active range of motion and allow the patient to continue strength training. While the patient was hypermobile through her adjacent fingers, there was a very slight hyperextension through the PIP joint of the operative finger compared to the contralateral side. However, this did not progress.
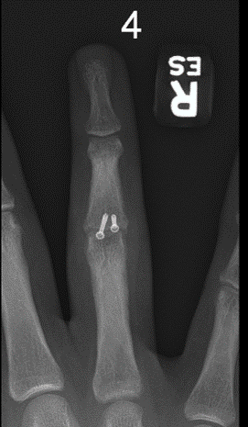
At six weeks, x-rays showed no evidence of hardware failure, anatomic alignment of the digit and callus formation around the fracture sites. On examination there was a slight lag at the DIP joint, which had been improving over previous weeks. Subsequently, there was a slight asymptomatic swan neck deformity present which hand therapy was focusing on to improve the Flexor Digitorum Superficialis (FDS) gliding. At this time the patient was cleared to return to contact ball work with no restrictions in the gym.
Below: Post-operative Images




DISCUSSION
In this instance, Prof. Couzens was able to treat a painful and debilitating injury for a young patient whose vocation requires the full use of her hand and fingers. With the NX Nail, Prof. Couzens was able to achieve definitive fixation through a percutaneous approach which gave the patient the best chance of returning to the field as soon as possible.
Product Resources
FO-003266-MM Version 2 April 2025