MEET THE SURGEON

Dr Andrew Mayo, MD
BSc(Med) MBBS(Hons) MEng FRACS FAOrthA
Subspecialist Upper Limb Surgeon Public and Private Practice Active in TeachingSpecial interest in hand, wrist, elbow, and shoulder trauma, degenerative conditions and instability
OVERVIEW
A 34-year-old left hand dominant wharf labourer presented to clinic after sustaining a closed injury to his left ring finger while playing indoor cricket.
Radiographs confirmed a displaced fracture of the head of his left ring finger middle phalanx. The decision was made to perform a percutaneous reduction and internal fixation using the NX Nail from Field Orthopaedics.
CASE INTRODUCTION
The patient is a 34-year-old left hand dominant wharf labourer who presented to clinic for evaluation of a closed injury to his left hand. The injury was sustained while playing indoor cricket when, during a catch, the ball collided with the end of his finger. Radiographs confirmed a displaced head fracture of the left ring finger middle phalanx.
CASE PRESENTATION
On examination, there was localised swelling and bruising of the digit. Flexion was limited due to swelling and rotational deformity was apparent. The skin had not been breached and the fracture had undergone emergency closed reduction at the time of the injury. Prior to this injury, the patient had no pain, disability or weakness in their hand.
Below: Pre-Operative Imaging
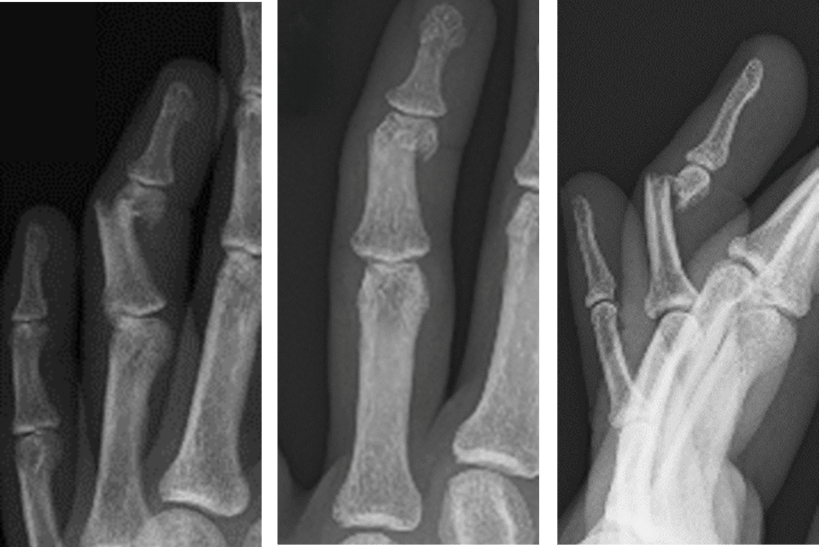
PRE-OPERATIVE PLAN
A closed reduction had been performed in the emergency room however the position was not anatomic and the patient had residual rotational deformity.
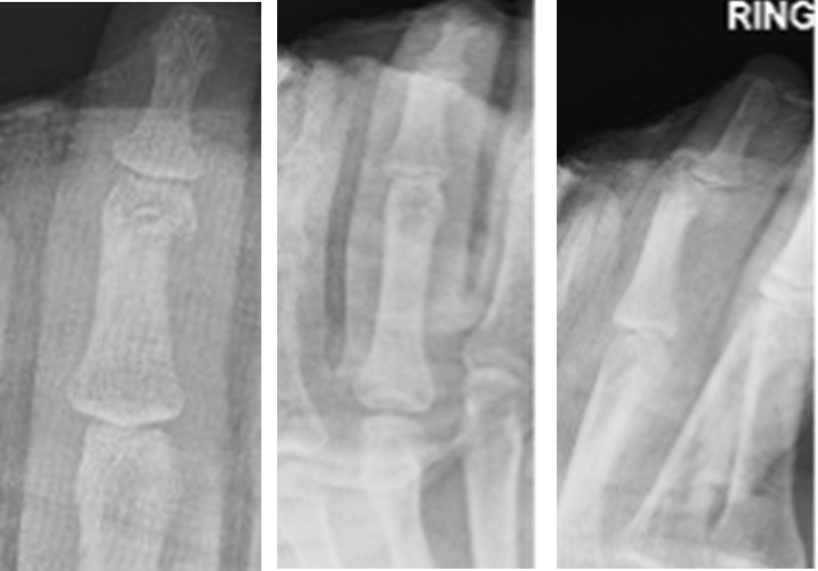
SURGICAL APPROACH
The patient presented for surgical fixation four days after the injury. Preoperative templating was performed and an estimate of canal diameter and corresponding nail size was obtained. The procedure took place under general anaesthetic with the patient in supine position.
Reduction
Closed reduction was achieved with traction and manual pressure. The distal interphalangeal joint was flexed to 90 degrees and, using the retrograde technique, an image intensifier (II) was used to identify the correct entry point and pass the K-wire into the medullary canal. Screw length was measured using the depth gauge and confirmed by holding the screw over the finger under II before insertion.
Templating
To confirm the diameter, the depth gauge was aligned with the borders of the isthmus of the phalanx under fluoroscopy. When templating, there was a slight lucency surrounding the depth gauge at the isthmus to allow the nail to easily pass through without making contact with cortical bone.
In this case, a 2.0mm NX Nail from Field Orthopaedics was used, ensuring subtle lucency around the threads.
Fixture
The corresponding cannulated drill bit for the 2.0mm NX Nail from Field Orthopaedics was placed over the K-wire and an insertion tunnel was drilled. The drill was passed beyond the isthmus and the position of the K-wire was maintained as the drill was removed.
There are two metaphyseal drills, the standard and the extended, to help prepare the bone in the shape of the implant head. The standard meta drill was used in this case.
After the appropriate path for the NX nail had been created, the length of the implant required was confirmed by using the depth gauge. The implant was inserted in a retrograde fashion over the K-wire with careful attention paid to ensure maintenance of reduction. Correct implant placement was confirmed with fluoroscopy and rotation of the finger carefully scrutinised and noted to be acceptable relative to the cascade of adjacent digits as well as the patient’s contralateral unaffected hand. Normal tenodesis of the digital flexors and extensors of all operative fingers was noted.

Closure
A single 5-0 nylon suture was used to close the wound. A dressing with non-adhesive gauze and a bandage was applied.
Postoperative protocol
The patient was referred to hand therapy for a protective mallet splint and encouraged to start full distal interphalangeal joint (DIPJ) range of motion immediately.
Follow Up
The patient was reviewed at two weeks, 6 weeks and 3 months post operation.
Two week review
Six week review
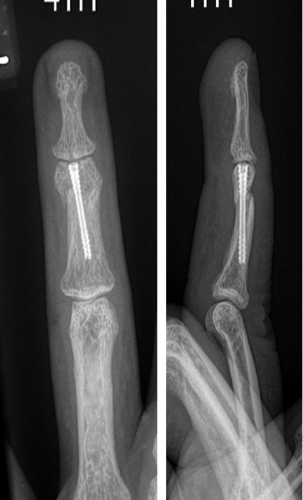
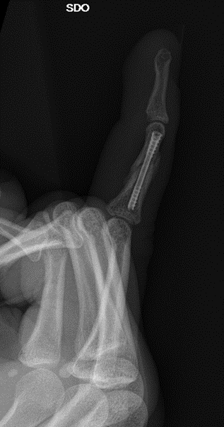
3 month review
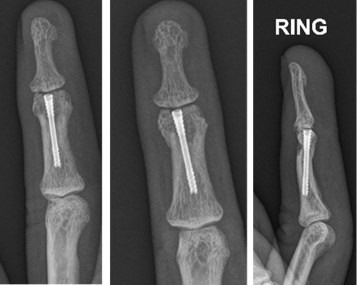
The patient was deemed to have completed a near full clinical recovery with approximately 10 degree loss of both active and passive flexion.
References
1. Field Orthopaedics. (2022). NX Nail Product Brochure. Brisbane, Australia: Field Orthopaedics.
2. Field Orthopaedics. (2023). NX Nail Long Surgical Technique. Brisbane, Australia: Field Orthopaedics.
FO-008136-MM Version 1 Apr 2023